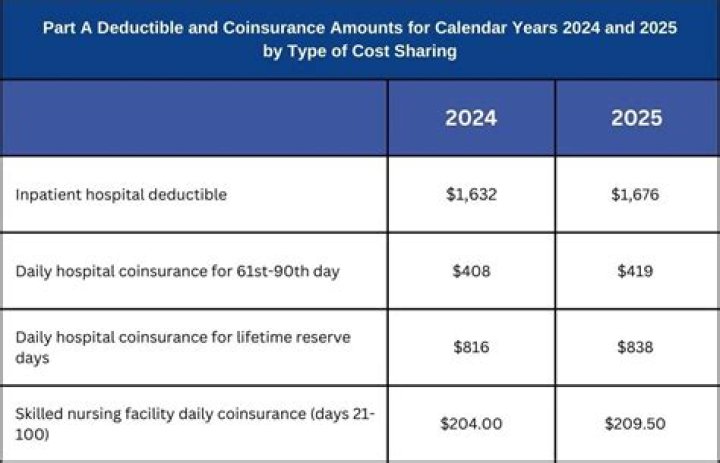
You must pay the inpatient hospital deductible for each benefit period. There’s no limit to the number of benefit periods. An amount you may be required to pay as your share of the cost for services after you pay any deductibles. Coinsurance is usually a percentage (for example, 20%).
What happens when Medicare hospital days run out?
Medicare will stop paying for your inpatient-related hospital costs (such as room and board) if you run out of days during your benefit period. To be eligible for a new benefit period, and additional days of inpatient coverage, you must remain out of the hospital or SNF for 60 days in a row.
How many days does Medicare pay for hospital stay?
90 days
Medicare covers a hospital stay of up to 90 days, though a person may still need to pay coinsurance during this time. While Medicare does help fund longer stays, it may take the extra time from an individual’s reserve days. Medicare provides 60 lifetime reserve days.
What happens when you reach your deductible?
After you pay your deductible, you usually pay only a copayment or coinsurance for covered services. Your insurance company pays the rest. Many plans pay for certain services, like a checkup or disease management programs, before you’ve met your deductible. Check your plan details.
How do you bill Medicare when benefits are exhausted?
In Form Locators 31-34 of the UB-04 Claim Form, indicate occurrence code “C3” and the date that Medicare Part A benefits were exhausted. Indicate the Medicare disclaimer code “M-7” on the Explanation of Medical Benefits form.
What are the 6 components of PDPM?
In the PDPM, there are five case-mix adjusted components: Physical Therapy (PT), Occupational Therapy (OT), Speech-Language Pathology (SLP), Non-Therapy Ancillary (NTA), and Nursing.
What is PDPM payment model?
The Patient-Driven Payment Model (PDPM) is the proposed new Medicare payment rule for skilled nursing facilities. Under PDPM, therapy minutes are removed as the basis for payment in favor of resident classifications and anticipated resource needs during the course of a patient’s stay. …
How many inpatient days will Medicare cover?
Original Medicare covers up to 90 days of inpatient hospital care each benefit period. You also have an additional 60 days of coverage, called lifetime reserve days. These 60 days can be used only once, and you will pay a coinsurance for each one ($742 per day in 2021).